The lack of recognition of occupational diseases is an important public health problem1,2,3 that will receive increasing attention by managed care organizations as they focus more resources on clinical preventive services. 4, 5, 6 Occupational diseases can be prevented by removing the worker from exposure or by making changes in the workplace. 7, 8 When occupational diseases are not recognized in the clinic, then the opportunity for prevention is lost.
The clinical recognition of occupational diseases is dependent upon an exposure history that can be efficiently and effectively performed. Such an exposure history can be viewed as a screening test.9 One of the requirements of a suitable screening test is that it can be quickly and easily administered.10
When screening for relatively rare diseases, the predictive value of a positive test will be low even if the test has fairly high sensitivity and specificity.11 A low positive predictive value means that the costs of investigating false positive results may exceed the benefits of the screening program. If this cost occurs in the form of time spent asking questions about false positive results on an occupational history questionnaire, then practitioners will realize that the activity is a waste of time, i.e., the costs exceed the benefits.
In order to improve the recognition of occupational diseases, an alternative method for screening is needed. This method should be quick and easy to administer and have high positive predictive value. There are two strategies for increasing the positive predictive value of a screening test.11 One is to target individuals in high risk groups. The other is to increase the specificity of the test. Both strategies reduce the number of false positives.
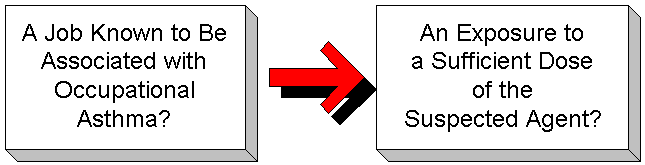
These strategies could be achieved by targeting patients belonging to certain occupations. For patients with asthma, only those belonging to occupations known to have higher risks for work-related asthma would be screened with specific questions for that occupation. The effect would be to break down the occupational history into two steps. The first step would determine if the patient's occupation was a known risk factor for the disease affecting the patient. The second step would determine whether or not the patient was exposed at a level sufficient to cause occupational disease on a more probable than not basis. Figure 1 illustrates this concept. Such a system of screening would take too much time to be implemented in a clinic with paper-based medical records. However, as computer-based patient record systems become more widely established during the next few years,12, 13, 14 and as clinical services become increasingly "evidence-based" and "population-based," the implementation of this kind of screening for occupational diseases will become feasible.

A number of studies have shown the capacity of computerized reminder systems and critiquing programs to improve clinical practice.16, 17, 18, 19, 20 In one recent study,21 a software program was used to critique the hypertension management of primary care physicians. After linking to the computer-based patients records (CPR), the program was able to review the coded data regarding blood pressure measurements, symptoms, laboratory results and medication usage to generate recommendations concerning drug information, diagnostic workup requirements and criteria for judging the efficacy of treatment. These recommendations compared favorably with the recommendations of physicians who independently audited the same medical records.
There are a number of reasons why occupational asthma was chosen as an occupational disease that could provide a useful model for the purposes of this study:
1) It appears that occupational asthma is now the most common occupational respiratory disease, at least in the materially developed parts of the world.22 Because of successful federal regulations and advances in industrial hygiene to reduce exposures by means of product substitution, improved engineering controls, and more effective use of personal protective equipment and medical surveillance, new cases of many of the "traditional" occupational diseases are rarely seen. However, the prevalence of occupational allergic disorders has not decreased, and there is evidence that the incidence of occupational asthma is increasing.23
2) The diagnosis of occupational asthma is very information intensive. There are over 200 known causal agents that have been associated with several hundred specific jobs.24, 25 Information about relative risks for different occupations is available from studies in the United States, Finland and the United Kingdom, e.g., incidence rates of 8 per million clerks and 1833 per million spray painters.26. 27, 28, 29
3) Unrecognized occupational asthma can result in significant patient morbidity. The natural history of immunologic occupational asthma (OA) can be diagrammed as:
onset of exposure > sensitization > OA > removal from exposure > persistence of asthma30
Each step is an opportunity to practice primary or secondary prevention (before asthma is diagnosed), or tertiary prevention (after asthma is diagnosed, but before work-relatedness is recognized).
4) Occupational asthma may be difficult to distinguish from non-occupational asthma, especially when the symptoms are not clearly related to work. Patients may present with recurrent attacks of cough and rhinitis. Patients with OA caused by low molecular weight compounds may experience isolated late reactions so that symptoms occur only at night.31 Symptoms may be exacerbated by nonspecific triggers such as cold air or exercise.32 Occupational asthma due to high molecular weight compounds is more likely to occur in atopic patients. These patients may have a history of pre-existent asthma caused by agents that are not work-related.33
In order to explore the opportunities for using CPR systems in primary care to improve the recognition of occupational diseases, a chart review of asthma patients was done at Group Health Cooperative of Puget Sound, Seattle, Washington. The objective of the study was to test the following hypothesis:
The currently used paper-based patient record system does not support effective screening for occupational asthma because it provides no means to target patients in high risk occupations nor to assist the physician in taking exposure histories relevant to those occupations.
Given the assumption that the CPR system has the features necessary to overcome the deficiencies of the paper-based system,34 then the corollary follows:
A computer-based patient record system could support effective screening of occupational asthma by helping physicians to focus on the patients that belong to high risk occupations and to take an exposure histories relevant to those occupations.
| Abstract | Slides | Introduction | Discussion |